Just after we got married, my wife and I embarked on an MBA (Masters of Business Administration). Along with teaching how the organs of business work, there were some interesting electives to choose from. One of the ones I chose was “Leadership and Motivation”. It provided guidance of how to lead people (as opposed to managing them), and how to motivate people. Obviously, in the context of an MBA, it was to help employees stay motivated to work on tasks deemed important to their employer, but I see parallels in the management of diabetes as well i.e. working on tasks deemed important for survival. For those not interested in the details, you can skip ahead to the tl;dr.
The 3C Model
The course was taught by Professor H.M. Kehr, formerly of UC Berkeley who created what is now called the “3C Model“; the Three Components Model.
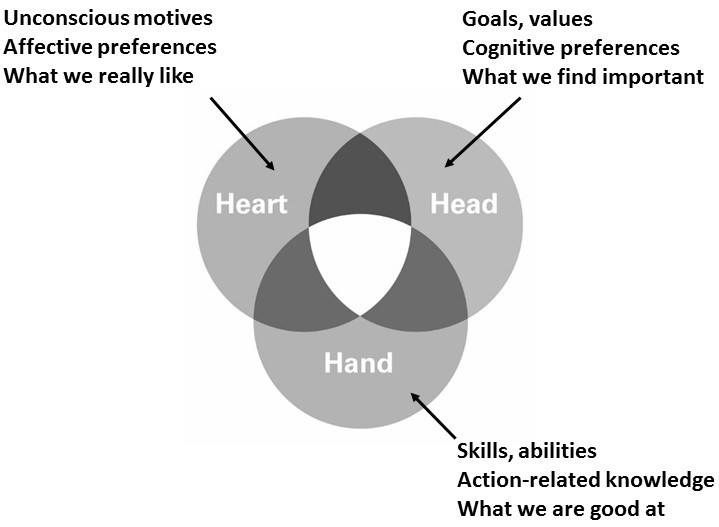
I find it easier to remember it as the “Head, Hearts, and Hands” model. While relatively simple, the model brought together various motivational models of the time e.g. Csikszentmihalyi and Rheinberg. In this case the head, heart and hands are:
- Head: Our logical thoughts regarding the task at hand
- Heart: How we feel about the task at hand
- Hands: Our ability to perform the task at hand
Other key concepts with the model are “volition” which, for the rest of us, is willpower and “flow”, a state of “effortless achievement”, which is sport is sometimes referred to as being “in the zone”. In short, when the head, heart, and hands are aligned, achievement is effortless.
Another key aspect of the model is the understanding that willpower is a finite resource which cannot be called upon indefinitely and, if pushed to its limit, leads to burnout. Burnout, of course, is a term familiar to many of us who manage diabetes meaning a complete abandonment of diabetes management.
Misalignment and Intervention
While alignment of the head, heart, and hands leads to a “flow state”, misalignment means willpower will be needed to achieve the task. For a task, such as diabetes management which is relentless, it is clear, without intervention, burnout is inevitable. Ideally, the intervention will either give the person a break from the task, allowing willpower to recharge, or make the amount of necessary willpower so small as to prolong burnout practically indefinitely.
Depending on which component is not aligned to the task, this dictates the kind of intervention to use.

When the head is the problem i.e. the person is emotionally aligned and has the skills, but there is a logical conflict, the person may need further convincing, have additional incentives put in place, or have the goals adjusted.
When the heart is the problem i.e. the task makes logical sense and they have the skills but it does not feel right, or they fear the task, emotional support, redesigning the approach, or focussing on the eventual outcome may help.
When the hands are the problem i.e. the person does not have the skills or knowledge to achieve the task, the answer may be education/training, coaching, or having others provide assistance.
Again, we start to see how this model could be overlay onto diabetes management and ensuring a specific approach is a good fit to the individual.
An Example of the Application of the Model
A classic example is the case of someone wanting to give up smoking. They know logically is makes sense (head), and may well have the skills to do it e.g. employing patches (hands), but their heart may not be in it or they fear failure. In this case we see suggested interventions which are often applied to help people give up smoking e.g. in New South Wales we have the ICanQuit web site and Quitline where people looking to give up smoking can call and get support and encouragement to help them on the path.
Application to Diabetes Management
The model provides insight into why intensive lifestyle interventions fail so often. While radical changes to diet or exercise in the management of diabetes frequently address the head and hands, the heart is almost always ignored and is the key point of failure. Very few of us deny the health benefits of exercise and most of us are capable of walking/running yet, like smoking, many of us fail to incorporate it into our lives. Simply put, our heart is not in it. Options to make exercise more palatable could be engaging a physical trainer to provide motivation (support), entering a charity fun run and then training towards the goal for the greater good (new motivators), or changing the type of exercise to something more enjoyable or aligned to the person’s lifestyle (redesigning the work).
In the case of Weight Watchers, the success rate is quoted at 11%. Even with intense coaching on top of lifestyle changes, one study showed remission for Type 2 was only achieved in 3.5% of participants. In the case of the Dr. Bernstein diet where the logic of the benefits of lowering dietary carbohydrates is sound (head), and there is no doubt, once the book is read, someone with Type 1 is equipped to undertake the program (hands), the majority of the strongest adherents, who literally commit to following the program to be part of the “international social group”, failed to meet the basic premise of sticking to 30g of carbohydrates per day. This is not the fault of any one program; the fact is changing habits and maintaining that change is hard and we need to consider the whole person to be successful. We must align the head, hearts, and hands for each person and provide the support that person needs. There is no “one size fits all”.
We also see this with diabetes technology. While the clinical studies speak at the benefits of, for instance, looping systems at improving outcomes (head), there may be a fear of using the technology due to a lack of skills/knowledge (hands) or the person simply does not like the idea of permanently wearing something on the body (heart). Professor Katharine Barnard-Kelly presents on this often at conferences and passionately believes “heart interventions” are effective at improving outcomes.
Professor Barnard-Kelly has also developed the Spotlight-AQ system which facilitates pre-clinic assessments to ascertain where interventions may be required e.g. the need for structured education (head/hands).
Putting the spotlight on my “Practical Diabetic Solution”, I think, if someone commits to replacing all meals, as I did, this would usually not be sustainable because the conflict with the heart e.g. no longer sharing food with family/friends would be simply too great. However, replacing non-social meals would not require the same level of willpower and the use of looping technology would greatly reduce the mental burden of daily management, assuming the person has the skills to use the loop (hands) and understand the benefits (head). To put it simply, the level of commitment and tool emphasis would be different for each individual, but a sustained improvement is better than one which fails to be maintained, however successful in the beginning.
How Can We Use This Model?
My vision is this could be used for self-assessment but also as a framework for the discussion between the health care team and the person with diabetes. For example, by considering why exercise may not work in the context of the three areas, a plan to address the disconnect can be intelligently devised. In the case of technology and medication, if one tool is not aligned, other tools can be considered instead with a closer fit, or other appropriate interventions considered.
tl;dr
The 3C Model of motivation, primarily used in the context of motivating employees, can also be applied to the management of diabetes and to frame conversations between health care professionals and their clients (people with diabetes).
The model focuses on three aspects of the individual, their:
- Head: logical thoughts on a diabetes management approach
- Heart: their emotional response to a diabetes management approach
- Hands: their skills and knowledge regarding a diabetes management approach
When all three are aligned with the approach, its use as part of the diabetes management plan is effortless. When one or more are not aligned, interventions are required to reduce the excessive need of willpower to use the approach which could lead to burnout. Interventions may include:
- Head: Education, adjustment to goals
- Heart: Support, redesigning of the approach
- Hands: Training, assistance
With a framework in place, it will be easier to identify appropriate interventions and optimise outcomes.
Great alignment of business strategy with the business of managing an insulin disorder.
LikeLiked by 1 person