I first read about incretin mimetics in Dr. Bernstein’s fourth edition of “Dr. Bernstein’s Diabetes Solution” published in 2011. He devotes nine pages to this class of drugs and it is a good place as any to describe what they do. It should be noted for those unfamiliar with Dr. Bernstein, his focus is on the treatment of Type 1 diabetes. While incretin mimetics are sometimes hailed as a ‘Type 2 drug’, they can be of benefit to diabetics of all Types as I will show in this blog.
From there I will update the information based on some peer reviewed papers from recent years (specifically relating to LADA) and the presentations at the recent EASD 2020 conference and then onto my own experience using them. As usual, there is the tl;dr at the end if you want the short version.
What Are Incretin Mimetics?
To understand the role of incretin mimetics, it is important to understand that beta cells produce, not just insulin, but also another hormone called amylin. Amylin is a ‘satiety’ hormone i.e. it makes you feel full. So, as the beta cells become damaged they are less able to produce this hormone. Amylin is released in response to the presence of ‘gut hormones’ in the blood, released when the gut is stretched. These ‘gut hormones’ are called ‘incretins’.
Based on all this, Dr. Bernstein suggests that diabetics of all persuasions are likely to not feel as ‘full’ as their non-diabetic counterparts. For me, this poses the question: “If someone who has impaired beta cell function cannot effectively regulate their eating, is it possible Type 2 diabetes and pre-diabetes causes obesity and not the other way around?” but that is a blog for another day.
At the time of writing his book, Dr. Bernstein describes incretin mimetics as being used to lower blood sugar levels after meals and for weight loss. We now know they have many more effects on the human body.
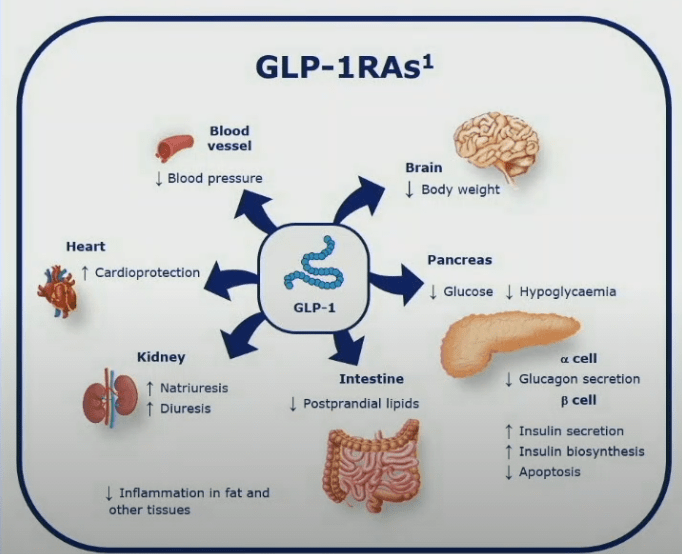
GLP-1 Receptor Agonists (GLP-1RAs) are one such incretin mimetic. As per the above we see, among other things, they can:
- Lead to weight loss (likely due to the increased sensitivity to feeling full)
- Lower glucagon secretion (meaning the liver releases less glucose into the blood)
- Stimulate insulin secretion and production (to process the food that is causing the stomach to feel full)
- Decrease beta cell apoptosis (this is the fancy name for programmed cell death. Cells in the body are given a countdown clock. When that clock reaches zero the cell destroys itself. Incretin mimetics tinker with that clock to extend the life of beta cells)
- Offer protection from heart disease
- Lower blood pressure
I should note that while these drugs do stimulate insulin production like, say, sulfonylureas unlike ‘sulfs’ the evidence shows this does not accelerate the demise of the diabetic’s honeymoon. My guess is the suppression of apoptosis counters the effect. Another possible explanation is, because the insulin is getting triggered earlier and harder, the blood sugars are not getting the opportunity to rise as high. Dr. Bernstein talks about how it takes more insulin to bring blood sugar down by a fixed amount when it is at a high level than when it is lower. So, the mimetics get the insulin out early when it is more effective and therefore the net production for a given meal is less.
Types of Incretin Mimetics
There are three types of incretin mimetics. These are:
- Amylin analogs: To my knowledge the only one on the market is Symlin (pramlintide). This is available by injection. I have not tried this one. EASD 2020 had a presentation on using it in a dual-hormone therapy (pumps with insulin and pramlintide) but the benefit of the additional pramlintide, in this context, was minimal.
- GLP-1 agonists (mentioned above): This is mentioned above with the associated effects. Until recently this was also only available via injection. Recently an oral version has been released (more of that later). I am currently on a once-weekly injection of this drug. Here are the six GLP-1s on the market at the time of writing.

- DPP-4 inhibitors: DPP-4s destroy GLP-1s in the body so this drug opposes that destruction and therefore, in principle, eliminates the need to inject GLP-1s. DPP-4s are available in an oral form and I took these for at least six months before moving to the GLP-1 agonists.
Contraindications and Side Effects
I will list some of the more common side effects but this list, like for most drugs, is far from exhaustive so discuss your specific history with your health care team to get a full picture of how well these drugs might suit your circumstances and complication risk profile.
Firstly, incretin mimetics slow stomach emptying so this can make gastroparesis (a condition not uncommon in Type 1s) worse. This slowing can also induce nausea. People on social media will be more than willing to tell you how incretin mimetics made them violently ill. For me, I feel mild nausea a day after injecting the GLP-1 agonist (akin to very mild car sickness) but felt no such effect when taking the DPP-4 inhibitors.
One side effect that was actually beneficial for me was constipation. As I also take Metformin, I have found the GLP-1 agonist and Metformin balance themselves out nicely giving me a lot of freedom I did not have when taking Metformin with the DPP-4 inhibitor. It is different for everyone though as GLP-1 agonists are also reported to have diarrhoea as a side effect.
One of the more serious side effects is the risk of reversible pancreatitis. I am informed pancreatitis is one of the most painful things you can experience and is usually characterized as a sudden, severe abdominal pain extending through the body from the back to the front. As the name suggests, stopping the medication reverses the condition.
LADA-Related Studies on DPP-4 Inhibitors
Given I am a Type 1 LADA trying to preserve my beta cells as long as possible and avoid the financial and mental stresses of insulin management, many of the studies I have earmarked, up to EASD 2020, are focussed on blood glucose management and beta cells preservation. Here are a few:
- Investigating optimal β-cell-preserving treatment in latent autoimmune diabetes in adults: Results from a 21-month randomized trial : n = 64 GAD-positive insulin-independent Type 1s. Insulin vs a DPP-4 inhibitor over 21 months. It was found that for patients with low GAD levels, both approaches preserved beta cell mass.
- Dipeptidyl Peptidase 4 Inhibitor Sitagliptin Maintains β-Cell Function in Patients With Recent-Onset Latent Autoimmune Diabetes in Adults: One Year Prospective Study : n = 30 LADAs. Half received insulin only and the other half received insulin and a DPP-4 inhibitor. Those who received the combined therapy produced similar levels of c-peptide as at the start of the study, compared to the insulin-only group who had significantly reduced c-peptide levels.
- Saxagliptin improves glycaemic control and C-peptide secretion in latent autoimmune diabetes in adults (LADA) : n = 2,709 GAD positive and negative diabetics (what I will call LADAs and Type 2s). Placebo controlled trial studying a DPP-4 inhibitor over 24 months. HbA1cs were reduced in both groups, LADAs had a reduction in fasting glucose and post-prandial glucose levels, beta cell function improved for both groups.
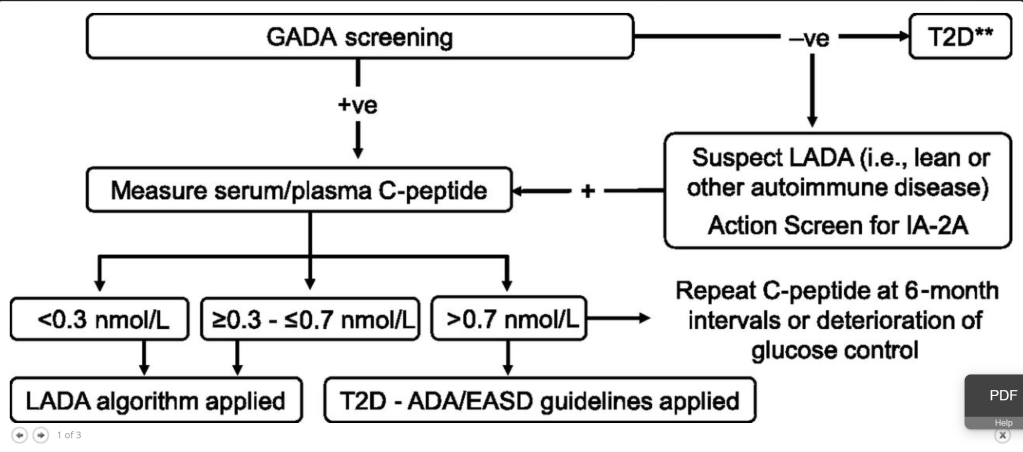
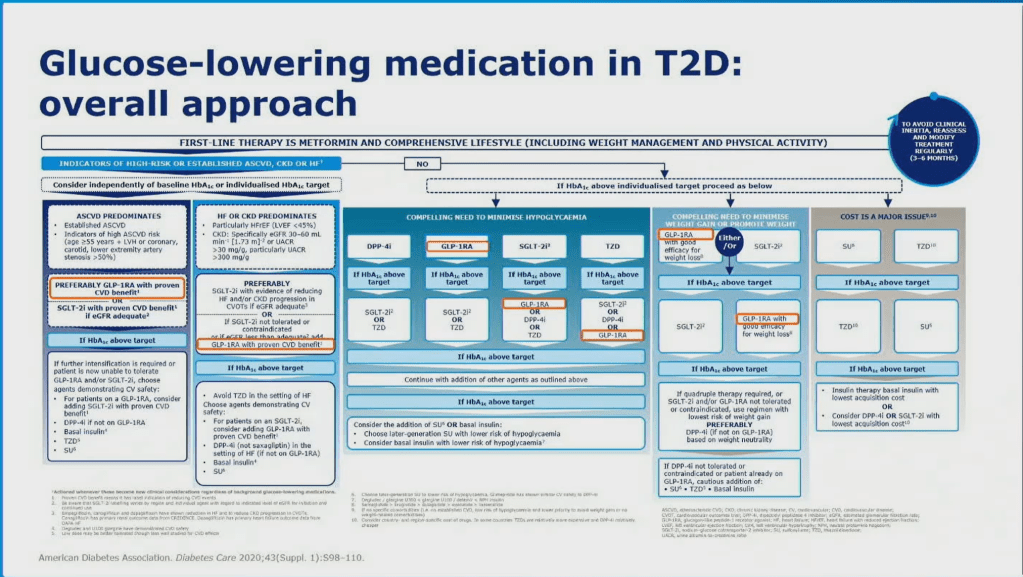
- Management of Latent Autoimmune Diabetes in Adults: A Consensus Statement From an International Expert Panel : Presents a flow chart for the treatment of LADA, depending on c-peptide levels. For high c-peptide levels, insulin is not recommended but a modified version of the Type 2 ADA/EASD guidelines are recommended which includes both DPP-4 inhibitors and GLP-1 agonists.
Presentations From EASD 2020
Tina Vilsbøll presented on Semaglutide, a new GLP-1 which can be taken as a once-weekly injection or as a once-daily oral pill, both being equally effective.

Juris Meier went into more detail as to the efficacy of the oral version, compared to other GLP-1 agonists, in Type 2s, showing it was more effective at reducing HbA1c.

The oral version of Semaglutide also compared favourably to the DPP-4 inhibitor Sitagliptin at doses above 3mg for Hba1c reduction and weight loss.


The downside was an increase in adverse reactions at the higher doses, compared to Sitagliptin.

So, if you are considering swapping out Sitagliptin for Semaglutide, understand that for a superior effect on HbA1c and weight loss you are also at a greater risk of those adverse effects.
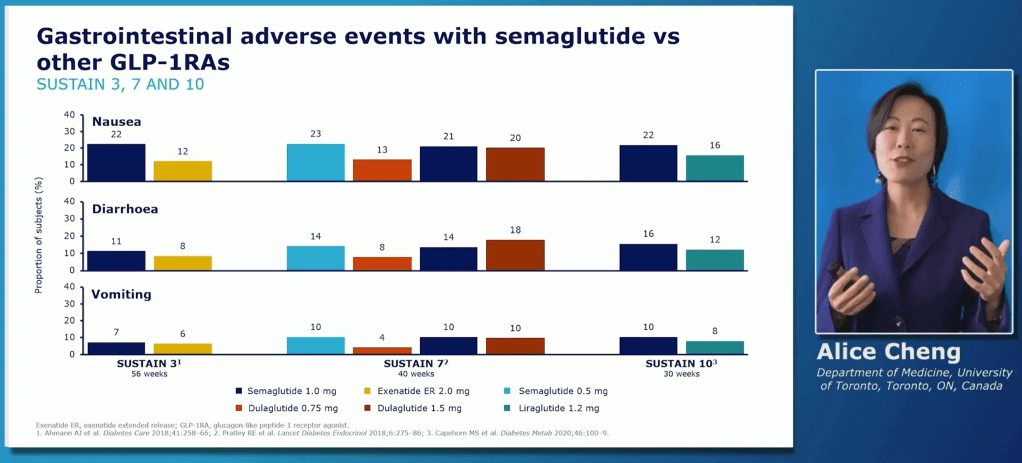
Alice Cheng showed how the injectable version compared favorably to both DPP-4 inhibitors and other GLP-1 agonists for reducing HbA1c and weight loss.

For adverse effects, Semaglutide was comparable to other GLP-1 agonists.
My Experiences With DPP-4 Inhibitors and GLP-1 Agonists
As mentioned, I have used both in an attempt to preserve my beta cell mass. For me, the DPP-4 Inhibitor had no side effects or, at least, any side effects were washed out by the ones from Metformin. The DPP-4 Inhibitor did nothing for me in terms of HbA1c reduction (although it is already in the mid-5% for this is not surprising), satiety, or weight reduction.
My experience with the injected GLP-1 agonists has been very different. Given the trouble I was having with Metformin, I halved that dosage but found the two drugs balanced each other nicely, as touched on before. I have lost five kilograms over a couple of months (I have it to lose) which I attribute to my significantly reduced appetite and improved sense of satiety. It is only now I realise it has been years since I actually felt full eating food and the GLP-1 agonist has given this back to me.
tl;dr
While traditionally considered a ‘Type 2 drug’, there can be benefits in incretin mimetics for all Types of diabetics. For all Types we have the general benefits of:
- Lowering blood pressure
- Lowering the risk of cardiovascular disease
- A sense of feeling ‘full’ which may be lacking in diabetics
- A lowering of HbA1c
- Weight loss (especially for the GLP-1 agonists)
For Type 2s, the benefits also include the lowering of blood sugar levels through the increased release of insulin after meals and supressed release of glucose from the liver.
For Type 1 LADAs there is growing evidence that incretin mimetics can help preserve beta cell function and prolong the honeymoon. Certainly the latest guidelines for managing LADA fully embrace incretin mimetics even if, formally, they are not approved for use in Type 1s.
In terms of side effects, incretin mimetics can cause stomach issues and nausea but, generally, these are mild and much less pronounced in DPP-4 inhibitors.
New innovations in incretin mimetics include:
- An improved once-weekly GLP-1 injection and
- An oral GLP-1 taken once-daily
While superior to similar products on the market in terms of their effects on HbA1c and weight loss, it comes at the cost of increased risk of side effects such as nausea, diarrhoea, and vomiting.
3 thoughts on “The Benefits of Incretin Mimetics For All Diabetics”