I had my six-monthly meeting with my Endocrinologist this week and it was clear the atmosphere was a little more formal than usual. Looking over my blood results he asked “Where do you want to start?”. Getting straight to the point I indicated the HbA1c number to which he replied “6.6%”.
This came as quite a shock as, for the five years since diagnosis, I had been 6.1% or less. The number had drifted up slightly in the last few results but this was quite the jump. “Well that’s it”, I concluded, “it is time to get onto the good stuff” which, in this case, meant insulin.
Set Your Goals and Limits Early
Back in November 2019 I had written a blog on what levels a person must maintain to limit damage and the risk of long term complications. My conclusion had been an HbA1c over 6.4% significantly increased the risk of complications and, once I reached this mark, it was time for insulin. That time had come.
I cannot recommend highly enough setting these kinds of personal limits early in your diabetes journey. Talk to your health team, review the literature as I did and create your own lines in the sand. When the time comes, they will serve you well because it is only natural to try and maintain the status quo when, in fact, change is necessary. Let your past self guide your present self so you can both look after your future self.
Grieving the Loss of Familiarity
I am a firm believer people go through grief when faced with significant changes in their life. The move to using insulin while not a big deal in itself, is such a change. While my other medications are to slow the progression of the disease and will no longer be needed in the future, the move to insulin is, in all likelihood, a permanent one.
The grief felt is, I believe, the grief of losing familiarity, of entering a new normal and the adjustments which come with it. In fact, the Kubler-Ross Grief Stages have been modified for chronic disease to cover this very concept.

In reviewing my HbA1c it was tempting to defend the result by considering the large error margin that is inherent in the HbA1c measurement (Denial) but, thanks to my regular reporting for my endo, I knew this result was consistent with the trend of my numbers heading upward and unlikely to be an outlier.
Without my line in the sand of 6.4% it would have also been tempting to give it another, say, six months, resisting my endo’s recommendation for insulin intervention and see where the numbers landed, doing my best to exercise more and eat less sugar in the interim (Pleading, Bargaining, and Desperation) but past Leon had prepared for this day allowing me to move past the second stage, reconciled by evidence over emotion.
There was a little Anger at myself for not doing more e.g. more exercise and less candy but, in reality, the immune system always wins. Five years of insulin independence was a remarkable achievement and it is mentally much healthier to focus on what was achieved than what was not.
There was also a little Depression that the inevitable had arrived along with small feelings of Loss of Self but, again, equipped with the knowledge that this was always going to happen helped me get past this. While there may still be some lingering feelings of this (while I write this it has been three days since I saw the endo), it is time to accept the next stage of my journey.
Acceptance and the Road Ahead
I had put on a sensor in the weeks leading up to the meeting with the endo so we had good information to guide us on where the high sugars were.
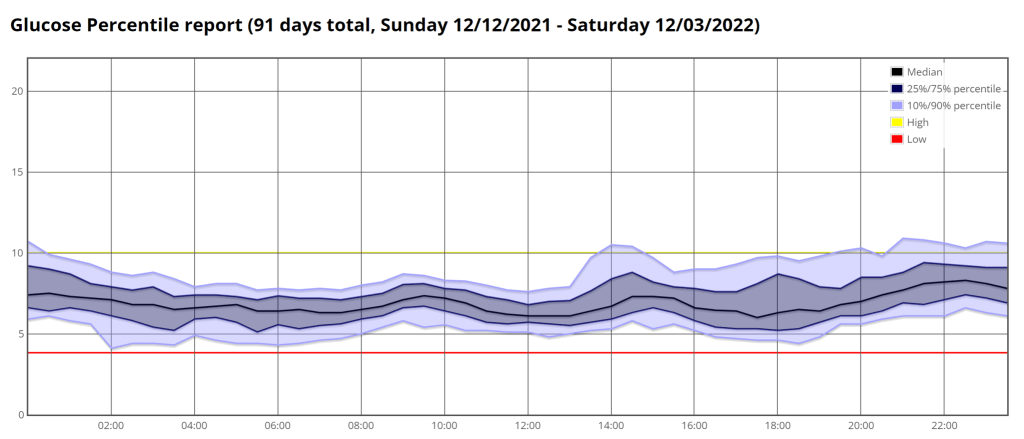
It is clear in the trace that from around 9pm at night my numbers go up and slowly drift down until morning. It is also clear that this drift sits around 7 mmol/L (126 mg/dL) and should probably be closer to 5 mmol/L. I remember when I was first diagnosed my blood sugars would sit in the 4s outside of meals but I have not been there for a very long time. This night-time elevation is where we decided to target the levels.
Long Acting Insulin
I spoke about the two main roles of insulin back in 2019. In short, if you are not eating, your levels should be reasonably flat and towards the bottom on the standard range e.g. 4.5-5.5 mmol/L (80-100 mg/dL). If the levels are not behaving like this, it is likely the body is struggling to keep the liver’s glucose release in check. For multiple daily injection, this is the role performed by long acting insulin.
As neither I nor my endo know exactly how much insulin is needed to flatten the overnight curve, we are starting conservatively: 2 units of Levemir taken at around 9pm and monitored once in the middle of the night (checking I am not too low), and once in the morning to see if I am between 4.5 and 5.5 mmol/L.
After one week I will see how it has gone and, if I am not getting down low enough, I will increase the dosage by another 2 units, monitor for another week, rinse and repeat.
There are a few long-acting insulins available but Levemir is useful for my specific purpose because it has peak activity for 12 or so hours which matches the period of time I need it for.

The New Normal
This is now my new normal; injecting once at night and for now, monitoring levels twice per day until I get the dosage right. My new goal is to reduce my HbA1c to a healthier level (sub-6% without hypos would be ideal) and if I can do this without the need for mealtime insulin, even better. Of course, if I continue to have an HbA1c above 6.4%, additional measures will be required. Again, the measures I have set for myself, informed by my own investigations and supported by discussions with my health care team, will guide me and allow me to keep a level head no matter what happens.
Sorry for this changes…. But also happy, that you are able to accept it and deal with it the way you do! I think, this is a healthy way to look at this disease. Although it might be hard, and I feel the anger and grief perfectly, to keep looking at the good achievements in the past and look forward and be grateful for the opportunity to use the medication we have is the power you have! Keep this power up! 😉
LikeLiked by 1 person
When I got to the point where my overnight glucose numbers were too high to be healthy, I stumbled upon a supplement that completely leveled out my glucose overnight, delaying my need for insulin for at least 2 years.
You might want to check it out: http://TypeADiabetic.com/supplement
I do not represent the manufacturer and do not make any money from referrals. It simply works for me so well that I bought a 4-year supply of it.
LikeLike
Thanks Jon. I’ll review the literature on the ingredients listed to see if there have been any studies.
As you know, I could take a nightcap to suppress my liver glucose production. This works because the liver sees alcohol, rightly, as a toxin which needs to be managed. My concern is a herbal supplement works in a similar way.
LikeLike
What I suggest is happening here is that one or more of the ingredients in this supplement are repressing hormones that are naturally released that trigger the liver to release glucose.
LikeLiked by 1 person